The NICU Collective The Future of NICU Care: How Federated AI is Training Life-Saving Models for NEC, BPD, and Growth Faltering
What if NICUs worldwide could teach powerful AI models to predict neonatal diseases without sharing a single patient chart? Federated AI is breaking down data silos to revolutionize how we predict NEC, BPD, and growth faltering.
Every day, clinicians in Neonatal Intensive Care Units (NICUs) ask three critical questions: Will this baby develop Necrotizing Enterocolitis (NEC)? How severe will their Bronchopulmonary Dysplasia (BPD) become? Are they at risk of growth faltering? Answering these questions requires predictive power. But to train an AI to predict these outcomes, you need massive amounts of data. Historically, that meant pulling patient records from dozens of hospitals into one central server, a process fraught with privacy risks, legal hurdles (GDPR/HIPAA), and competitive resistance.
NICUs generate incredibly sensitive, high-dimensional data. A single preemie’s vital signs, nutrition logs, and respiratory support settings are protected by the strictest privacy laws. This creates a paradox: the data exists to save lives, but we cannot legally or ethically move it to a central location to train the models.
Conditions like NEC or BPD develop over days or weeks, and they are perfect candidates for a revolutionary technology called Federated Learning. Think of Federated Learning as a “study club” for NICUs, rather than a library.
- The Old Way (Centralized): Every NICU has to send copies of their patient books to one big central library. That means paperwork, anonymising patient data, ethical approvals, and hoping nothing gets lost or leaked along the way. The effort involved means notebooks take a long time to be written, and some hospitals just don’t bother joining in.
- The Federated Way: The librarian sends a blank notebook to each NICU. Each hospital writes down what they learned from their own patients, without showing the librarian the actual patient charts. The librarian combines the lessons (the model weights) and sends back a smarter notebook. The patient data never leaves the hospital firewall.
At Preemie Health, we are deploying Federated AI to solve the problem of “rare event” prediction. A single NICU might only see 5 severe NEC cases a year. This is not enough data to train a reliable algorithm. But 50 NICUs together? That is a dataset powerful enough to detect the subtle vital sign dips and feeding intolerance patterns that precede NEC.
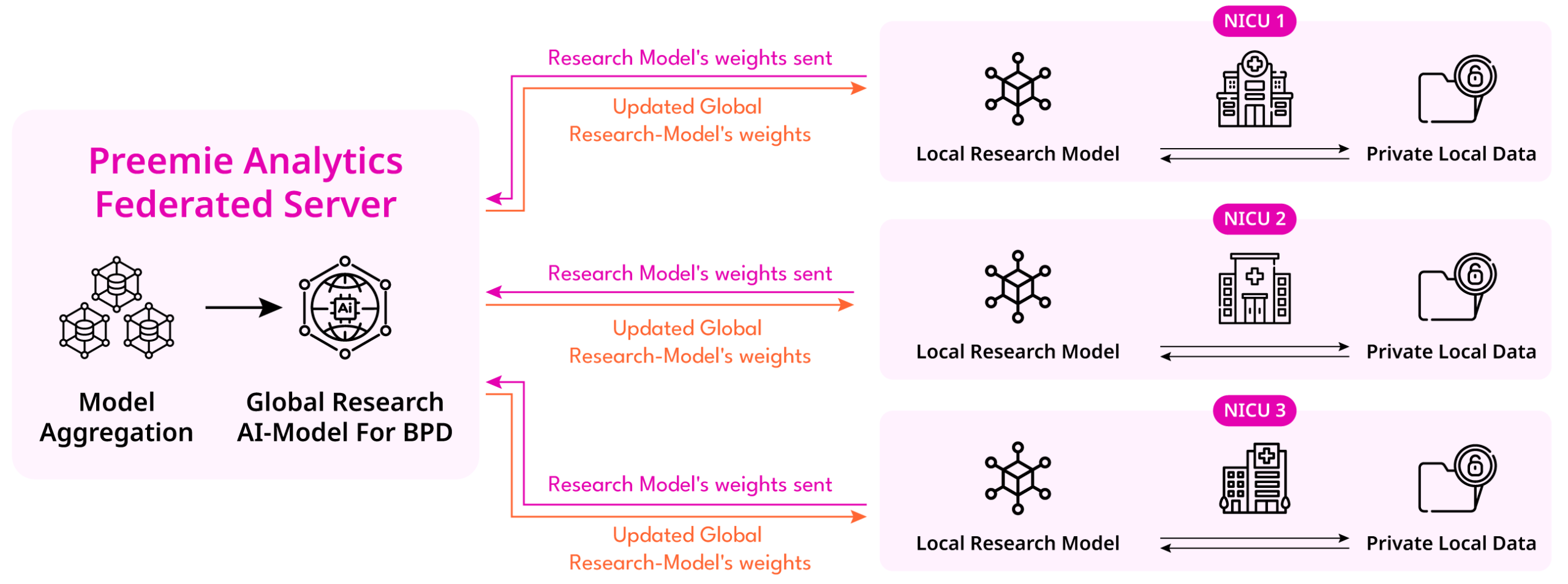 Here is how the math works, a case study:
Here is how the math works, a case study:
- Local Training: Our software, Preemie Analytics, runs models inside each NICU’s secure server. The model learns to predict preterm disease severity based on local gestational age, birth weight, and other clinical parameters.
- Weight Sharing: Instead of sending patient data, the NICU sends “model updates” (mathematical gradients) to Preemie’s central cloud.
- Aggregation: The central server aggregates these updates.
- Global Insight: The resulting global model is not biased to one hospital’s parameters alone, and it is significantly more accurate than the predictive model from any single hospital. This creates a generalized, robust predictor for a specific disorder.
Why Is This a Breakthrough in Neonatal Care?
- Learning the “Long Tail” of BPD
BPD isn’t a single disease, it is a spectrum. Centralized models often miss the rare phenotypes. Federated AI allows us to train models on the “long tail” of BPD presentations across diverse populations without exposing a single chest X-ray. - Predicting NEC Before the Explosion
NEC can progress from suspicion to surgery in hours. Federated models allow us to detect the pre-NEC phase, subtle changes in abdominal girth and gastric residuals, by learning from thousands of historical cases where NEC almost happened but was averted. - Solving Growth Faltering with Nutrition Logs
Growth faltering is often a data hygiene problem. One hospital measures z-scores weekly; another uses WHO charts. Federated Learning allows us to normalize these disparate data types. The model learns that relative deceleration in weight velocity is a universal risk factor, regardless of how the hospital formats its log.
Preemie is building a future where a NICU in rural or low-resource settings benefit from the collective wisdom of top-tier academic centers, not from a single, frozen model, but from a living system. Every day, fresh, deidentified data from participating NICUs continuously enriches the research models. Those models are then periodically revalidated by regulators such as the FDA to become the newest clinical decision support tool. This means a baby with borderline growth stats gets flagged for intervention based on the most current evidence, drawn from thousands of recent cases across the globe, and the system evolves as populations, health trends, and care practices change. Patient trust is never violated, and clinical guidance never goes stale.
We are building a future where a rural NICU benefits from the collective wisdom of a top-tier academic center. Where a baby with borderline growth stats gets flagged for intervention because the AI learned from 10,000 similar cases across the globe.
Ready to Join our NICU Collective? If you are a NICU leader or researcher interested in collaborating on models, contact us today.